Bassett Community Health Navigation
Health Home Care Management
What is a Health Home?
A Health Home is not a place; it is a group of health care and service practitioners working together to make sure you get the care and the services you need to stay healthy. Once enrolled in a Health Home, you will be assigned your own Care Manager / Care Navigator. These services are provided at no cost to members.
What Can a Care Manager / Care Navigator Help With?
Health Home Care Management is a service that is free to qualifying Medicaid recipients who need additional assistance with:
- Linking to any needed practitioners such as doctors, dentists, specialists, etc.
- Applying for and/or appealing SSI/SSDI and benefit maintenance.
- Coordinating hospital admissions and discharges including outpatient procedure, and assisting with any services needed after discharge.
- Linking to any available programs, services, and funding sources needed.
Who Are our Care Management Partners?
Bassett Community Health Navigation has several partners that work within the Health Home providing Care Management / Care Navigation services. The following are our partners:
- Bassett Community Health Navigation
- Rehabilitation Support Services
- Schoharie County Mental Health
- ICAN
Who is Eligible for Services?
Those eligible for Health Home services must have active Medicaid, and one of the following:
- Two or more chronic conditions
- Serious mental illness
- HIV / AIDS
- Sickle Cell Disease
What Areas Do You Serve?
We currently serve the following counties:
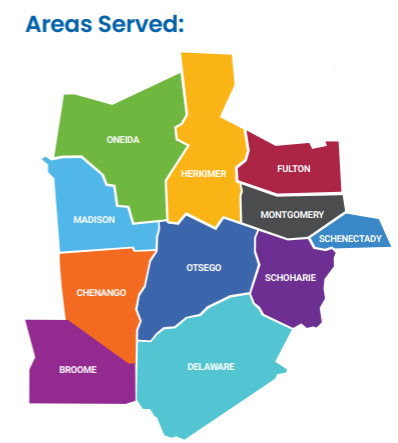
- Broome
- Chenango
- Delaware
- Fulton
- Herkimer
- Madison
- Montgomery
- Oneida
- Otsego
- Schenectady
- Schoharie
